Proton Therapy
In the ever-evolving landscape of medical advancements, proton therapy stands out as a beacon of hope for patients battling cancer. This innovative form of radiation treatment promises greater precision and fewer side effects compared to traditional methods. But what exactly is proton therapy, and how is it being applied in modern medicine? In this detailed blog post, we’ll dive deep into its mechanics, benefits, applications, and more, shedding light on why it’s gaining traction worldwide.
The Origins and Invention of Proton Therapy
The story of proton therapy begins with a visionary physicist. In 1946, Harvard’s Robert R. Wilson proposed the idea of using accelerated protons for cancer treatment, recognizing their potential to deliver radiation more precisely than X-rays. Though the concept was groundbreaking, it took decades for it to reach clinical practice—the first hospital-based proton therapy center opened in 1990 at Loma Linda University Medical Center in Southern California, marking a pivotal moment in oncology. Today, this “next great frontier” in cancer care continues to evolve, offering safer and more accurate alternatives to conventional radiation, as highlighted in discussions on its transformative potential.
For more on its historical journey and why it’s considered a buzzword in oncology, check out this insightful overview: The Next Great Frontier of Cancer Treatment – Proton Therapy.
What is Proton Therapy?
Proton therapy, also known as proton beam therapy, is an advanced type of radiation treatment that uses beams of protons—positively charged particles from hydrogen atoms—to target and destroy tumors. Unlike conventional radiation therapy, which relies on X-rays (photons), proton therapy leverages the unique physical properties of protons to deliver energy more precisely to the tumor site. This precision stems from a phenomenon called the Bragg peak, where protons deposit most of their energy at a specific depth in the tissue, stopping abruptly afterward with minimal exit dose to surrounding healthy areas.
Traditional X-ray radiation, in contrast, releases energy along its entire path through the body, including before and after the tumor, which can harm nearby healthy tissues. Proton therapy minimizes this by focusing the maximum dose exactly where it’s needed, potentially reducing side effects and allowing for higher doses to the tumor itself.
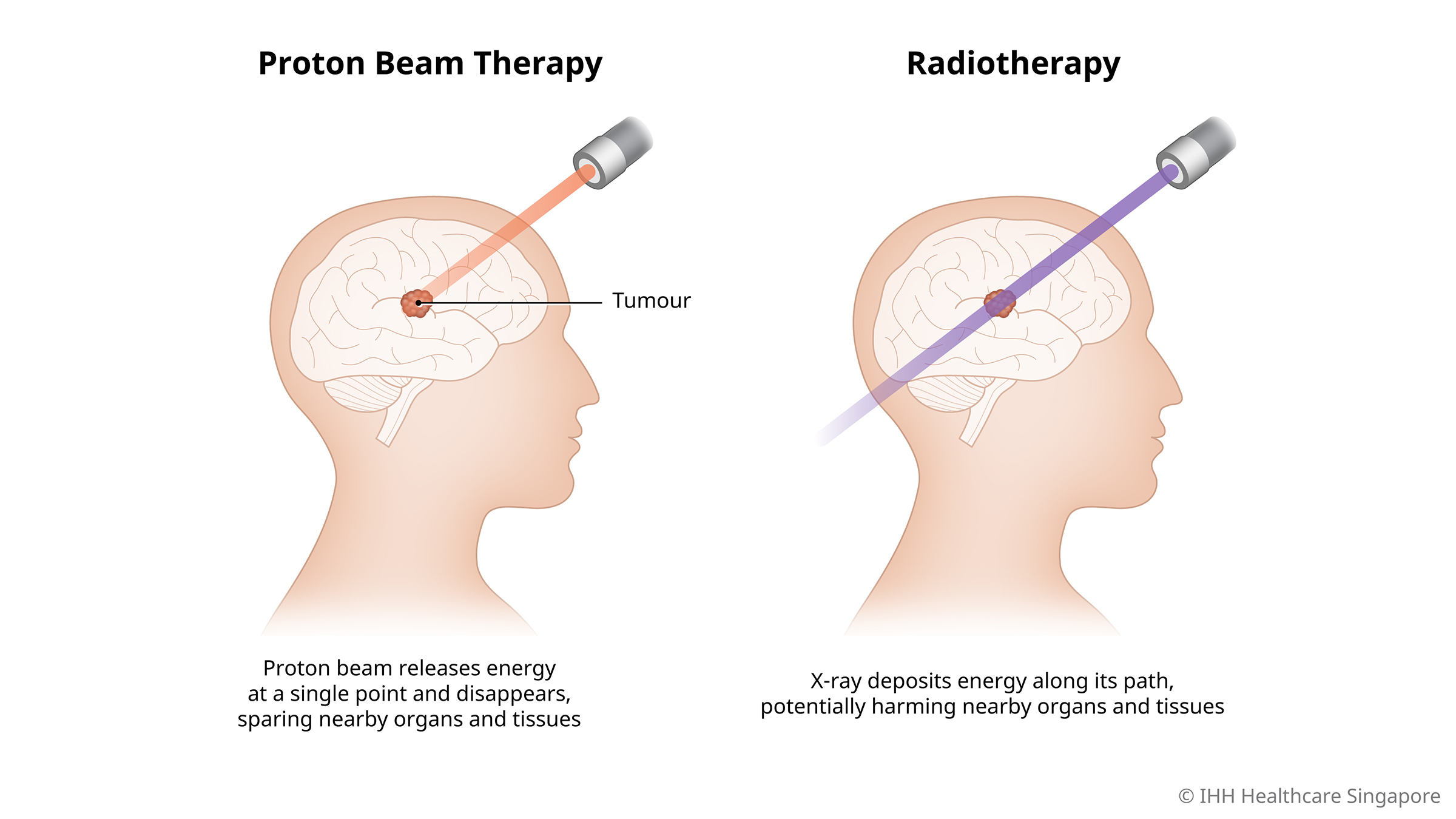
Image Credits: mountelizabeth.com.sg
Proton Beam Therapy | Mount Elizabeth Hospitals
How Does Proton Therapy Work?
The process begins with a particle accelerator, such as a cyclotron or synchrotron, which strips electrons from hydrogen atoms to produce protons and accelerates them to high speeds—up to about 60% the speed of light. These protons are then directed through a beam transport system into a treatment room, where a large rotating device called a gantry focuses them into a narrow beam (about 5 millimeters wide) aimed at the tumor from multiple angles.
Doctors adjust the energy of the protons to control how deep they penetrate, ensuring the Bragg peak aligns with the tumor’s location. For larger or irregularly shaped tumors, techniques like pencil beam scanning are used, where the beam sweeps across the target layer by layer, creating a spread-out Bragg peak (SOBP) to cover the entire volume. This allows for intensity-modulated proton therapy (IMPT), which optimizes the dose distribution for maximum tumor control and minimal healthy tissue exposure.
Treatment sessions are outpatient and typically last 15-45 minutes, with the actual beam delivery taking only a few minutes. Patients lie still on a table, often secured with custom molds or masks, while imaging like CT or X-rays ensures precise alignment before each session. The therapy team monitors from an adjacent room, and patients feel nothing during the procedure—no pain, heat, or sensation.
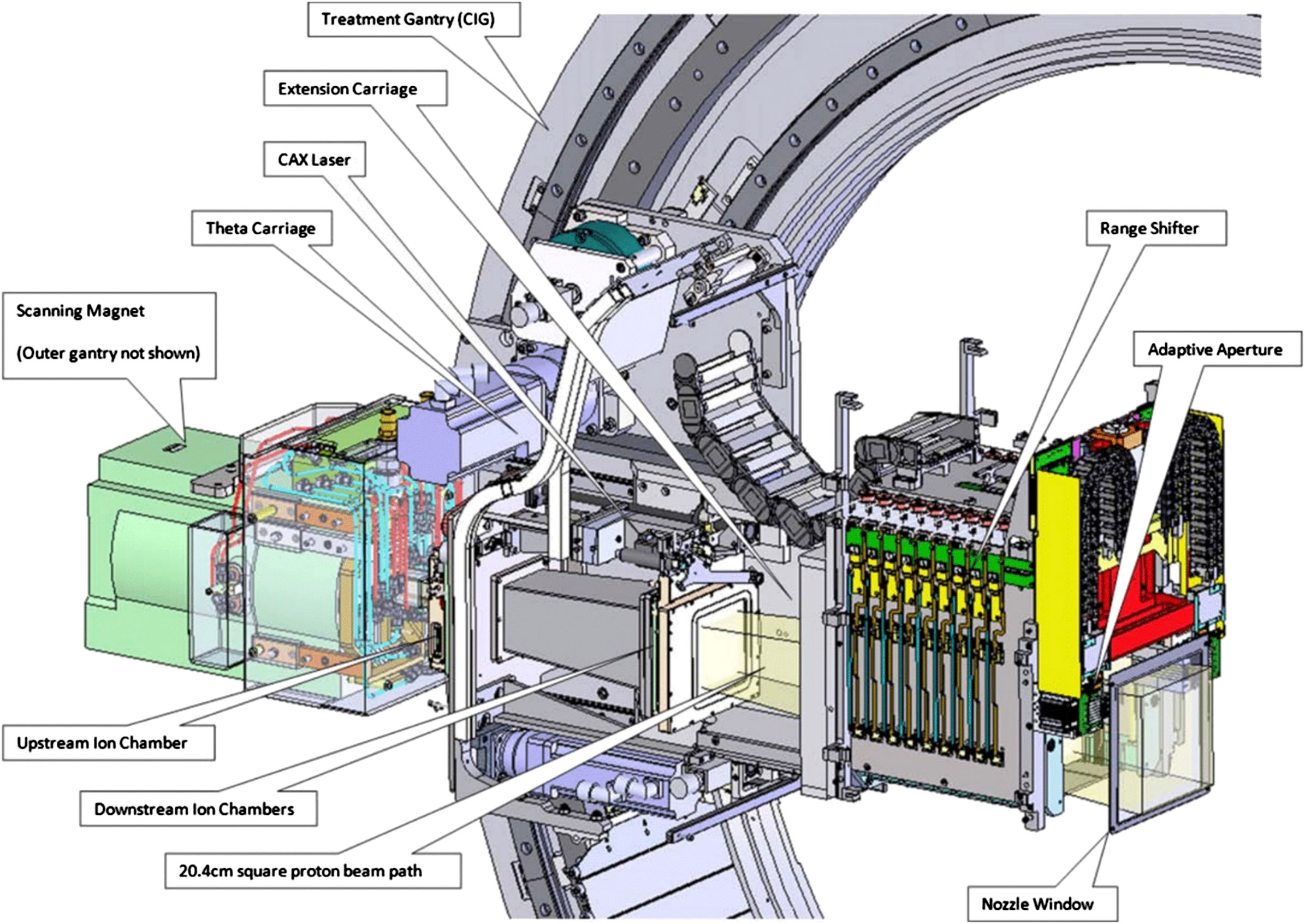
Image Credits: frontiersin.org
Applications of Proton Therapy
Proton therapy is primarily used to treat both cancerous and noncancerous (benign) tumors, often in combination with surgery, chemotherapy, or other therapies. Its precision makes it ideal for tumors near critical structures, where sparing healthy tissue is crucial. Common applications include:
- Brain and Central Nervous System Tumors: Effective for brain tumors, pituitary gland tumors, and those at the base of the skull or spine, reducing risks to neurological functions like vision, hearing, or cognition.
- Pediatric Cancers: Particularly beneficial for children, as it lowers the risk of long-term side effects like growth disorders, secondary cancers, and developmental issues. It’s used for medulloblastoma, retinoblastoma, and other childhood neoplasms.
- Prostate Cancer: Allows higher doses with less impact on surrounding organs like the bladder and rectum, potentially reducing urinary and bowel side effects.
- Breast Cancer: Especially for left-sided cases, it minimizes radiation to the heart and lungs, lowering cardiovascular risks.
- Head and Neck Cancers: Targets tumors while protecting salivary glands, eyes, and nerves to preserve quality of life.
- Other Cancers: Includes esophageal, liver, lung, pancreatic, lymphoma, sarcoma, and eye melanomas. It’s also used for recurrent tumors or reirradiation scenarios.
Ongoing clinical trials are exploring its efficacy for additional cancers, such as gastrointestinal malignancies and hepatocellular carcinoma. By 2019, over 200,000 patients worldwide had received proton therapy, with numbers continuing to grow as more centers open.
Proton Therapy in India: Current Landscape and Accessibility
While proton therapy’s global adoption is accelerating, its rollout in India is a story of rapid progress amid challenges. As of November 2025, the country boasts only two fully operational centers, but with three more in the pipeline, access is set to expand dramatically. This development is crucial for a nation with a high cancer burden, where cost and location have historically limited advanced care.
Operational Centers
- Apollo Proton Cancer Centre (APCC), Chennai: India’s pioneering facility since 2019, this JCI-accredited center has treated over 2,500 patients from 147 countries. Costs range from ₹10-30 lakh per course.
- Tata Memorial Centre (TMC) – ACTREC, Navi Mumbai: The first public-sector site, operational since August 2023, it has served 541 patients by August 2025, with 60% treated for free and others at subsidized rates (around ₹10 lakh).
Upcoming Facilities
- AIG Hospitals, Hyderabad: A ₹800 crore investment for a Proteus®ONE system, expected soon in a new 300-bed oncology center.
- Apollo Hospitals, Hyderabad (Jubilee Hills): Set for FY2028, with capacity for 350 patients annually.
- Apollo Hospitals, Gurugram: Part of a larger expansion, targeting completion in the next four years.
Importantly, many hospitals advertise advanced radiation but lack true proton capabilities—facilities like Max Healthcare, Medanta, and Fortis offer excellent alternatives like IMRT but not proton beams. For a complete directory, see: Complete List of Hospitals with Proton Therapy Treatment in India.
Advantages and Disadvantages
Advantages
- Precision and Reduced Side Effects: Delivers up to 60% less radiation to healthy tissues, leading to fewer acute and long-term side effects, such as fatigue, skin irritation, and secondary cancers.
- Higher Tumor Doses: Enables dose escalation for better tumor control in hard-to-treat areas like the skull base or spine.
- Safer for Sensitive Areas: Ideal for protecting vital organs and functions, especially in children and near the heart, brain, or reproductive organs.
- Outpatient and Non-Invasive: No radioactivity post-treatment, allowing normal activities to resume immediately.
Disadvantages
- Limited Availability: Only about 89 centers worldwide as of 2023, often requiring travel.
- High Cost: Equipment and treatment are expensive (up to 2.4 times traditional radiation), and insurance coverage varies.
- Longer Planning Time: Requires detailed simulation and quality checks, delaying start compared to photon therapy.
- Not Universal: May not offer significant benefits for all cancers, like some prostate cases affected by organ motion.
Side Effects and Preparation
Side effects are generally milder than with traditional radiation but can include fatigue, skin redness, hair loss in the treated area, and site-specific issues like headaches or digestive problems. They often develop gradually and depend on the treatment site and dose.
Preparation involves a multidisciplinary team conducting imaging (MRI/CT) to map the tumor, creating custom immobilization devices, and planning the dose with computer simulations. Patients may receive temporary markers or small tattoos for alignment.
The Future of Proton Therapy
With advancements like compact single-room systems and FLASH therapy (ultra-high dose rates in seconds to further reduce side effects), proton therapy is becoming more accessible and effective. Research continues to refine its applications, potentially expanding to more cancer types and improving outcomes.
In conclusion, proton therapy represents a significant leap forward in personalized cancer care, offering targeted treatment with fewer compromises on quality of life. If you’re facing a cancer diagnosis, consult with specialists to see if it’s right for you—precision medicine like this could make all the difference.
